Losing Hair, Growing Faith
October 02, 2018Cancer is a disease in which attitude is everything. (M. Barry)
We do not only fear cancer, but we also fear its treatment. And, this fear is very valid because treatment is definitely not a walk in the park. Chemotherapy exhausts me. I am fatigued, I am in discomfort, and I cannot understand my body the days following a session. I am not only physically down, but also mentally, emotionally, and spiritually weakened. When I am in bed and dark thoughts—hopelessness, powerlessness, or despair—enter my mind, I recite Psalm 23 repeatedly and tell myself that these dark days (about 3 to 5 days after a session) shall pass. As of this writing, I have been to 4 chemotherapy sessions that are 21 days apart and the journey has not been easy.
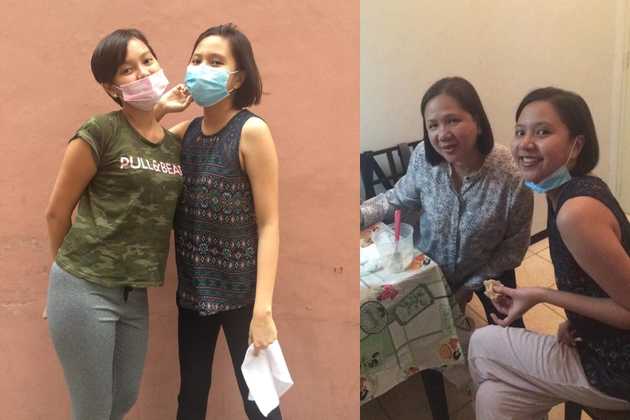
The moment I stepped in to the building of our rented place in Manila after my first chemotherapy session, I vomited. The following days were my first dark days. I mostly stayed in bed. I didn’t have the energy to move nor the appetite to eat so my mother had to spoon-feed me. It was only the beginning and I was already miserably thinking how others get through this. When the dark days were over, I cut my hair shorter in anticipation of hair loss, the most visible side effect of chemotherapy, and in support, my mother and sister cut theirs shorter too. I started losing my hair during the third week after my first chemotherapy session. It began like a normal hair fall until it became really bad. I was losing my hair in clumps when I showered and when I combed it even with just my fingers. Hair strands also did stick everywhere—in my pillows, in the couch, and even in the wall I just leaned on. I had to wrap my head because picking up all the fallen hair strands was tedious. My hair eventually thinned out and bald patches were formed. However, losing my hair was just the tip of the iceberg.
A week prior to my scheduled second chemotherapy session, July 30, my tooth was aching. I saw a dentist on July 23 and she confirmed that I had an infected molar, which was beside an impacted wisdom tooth. It was unfortunate how careful we were to avoid infection—we even wore masks at home—only to be infected by my own body. I needed medical clearance for tooth extraction so I saw my cardiologist on July 25. He told me and my parents to weigh the risks of bleeding and pulmonary embolism—I am taking anticoagulant medication, a potent one that does not have an antidote, for my thrombus which places me at high risk for bleeding and if I undergo any procedures, this medication has to be stopped for 48 hours, which would then increase my risk of pulmonary embolism. He said that this might need another multidisciplinary or family meeting and bluntly told me to ask my oncologist about my life expectancy. I was discouraged. I went to my oncologist, explained about my tooth, and asked about my life expectancy. She answered, “Honestly, I do not know. I do not hold your life. You do not hold your life. I even do not hold mine. I really do not like answering this type of questions because it doesn’t help. If the numbers are at 98% versus 2% and only the 2% define our chances, we still hold on to the 2%. In our field, we want to see the glass half-full and not half-empty. We always hope.” I was comforted. I was reminded that the Lord holds my life in His palm (John 10:28).
My oncologist admitted me that day, placed my chemotherapy schedule on hold, and referred me to a dental surgeon and Infectious Disease Specialist (IDS). My White Blood Cell (WBC) count was only at 1.10 (Normal Range: 4.50-10.00 x109/L) so I was given Granulocyte Colony Stimulating Factor (GCSF) subcutaneously and was recommended for dental procedures. My cardiologist was also on board. He stopped my oral anticoagulant and overlapped it with an intravenous one. On July 27, I was wheeled in to the dental clinic in the afternoon for a root canal therapy and to the Operating Room in the evening for a tooth extraction. Both procedures were done successfully and without complications so I was shifted back to my oral anticoagulant. My WBC count also increased to 3.58, which resumed my chemotherapy schedule. I was again in awe of God’s power and glory, which I witness more when I am weak and not in control.
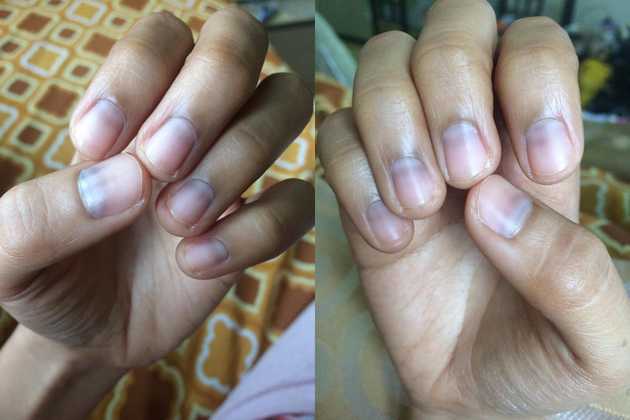
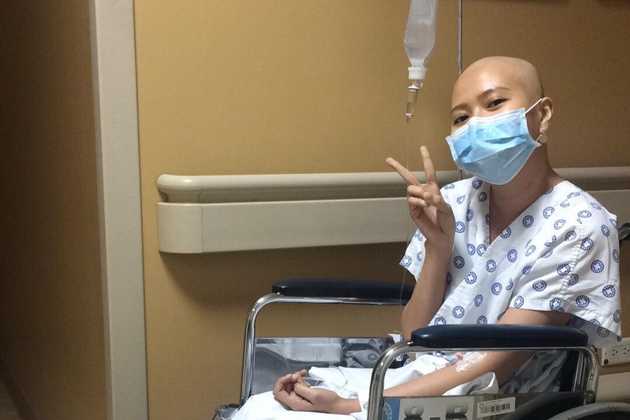
After my second chemotherapy session, I went to the salon to have my hair shaved. I thought I would cry over being bald but I didn’t. I was instead relieved from the stress of losing my hair in clumps. And, I felt lighter. Aside from the hair loss, my skin and nail beds started turning dark. Previous intravenous insertion sites were also slow to heal.
On August 20, I was admitted again because I had to undergo some diagnostic procedures prior to my third chemotherapy session. I first underwent CT scan of the chest and the upper abdomen in the afternoon. When I was wheeled in to the Radiology Department, my intravenous cannula was dislodged and they had a hard time reinserting that they had to call two resident doctors. And, during the procedure, I was worried because I only felt the side effects—metallic taste and warmth—of the contrast on the left side of my body. My worry worsen in the evening when I underwent echocardiogram and the technicians had difficulty on visualizing two of my heart chambers. They explained that it may be because of my thin frame. But, I was not comforted, especially when I was wheeled in again the following day to the Cardiovascular Unit for additional views of my heart. Also on the following day, I underwent CT angiography of the neck vessels.
On August 22, my worries were eased. My CT scan results were favorable. Although the tumor recurrence did not shrink, it did not enlarge. There was also regression of the metastases. And, even though extensive thrombosis was still seen on my right neck and upper chest veins, collateral veins were already formed. My oncologist concluded that the initial combination of chemotherapy drugs was working so my third chemotherapy session was then started once I was cleared from my cardiologist who reported that my echocardiogram result was fine. However, my joy was short-lived.
In the evening, an interventional radiologist visited me and explained that he would not recommend stenting of my Superior Vena Cava (SVC), an option to alleviate my SVC syndrome that my cardiologist mentioned we have yet to see possible, because even if a stent would be miraculously inserted, I will still be on anticoagulant therapy to maintain the patency of the stent. And, the collateral veins formed had already been enabling blood from my upper body to drain back to the heart. Hence, he recommended that it is better not to touch my occluded SVC and that I just have to take anticoagulant medication forever. He also emphasized its contraindications, such as contact sports, and advised me to avoid contraceptives and pregnancy, which increases the risk of developing blood clots. I prayed to the Lord that I do not have to undergo stenting and He answered it. But, I was struck and sad of the other things that the interventional radiologist said. When my oncologist came, she appeased me, saying that forever is a long time. She also opened up about the option of continuing treatment in Cagayan de Oro because really there is no place like home. When I asked about how many more sessions I need, she said that it depends because with Stage 4 cancers, treatments such as chemotherapy is palliative. She mentioned the 4 reasons patients at this stage may choose to stop undergoing chemotherapy: the patient cannot tolerate the side effects, chemotherapy is not working, the condition is not improving nor worsening, or the patient simply chooses not to. But, I thought of a fifth reason: The patient is healed. Even when confronted with the dreadful word palliative, my trust in the Lord remained steadfast (Psalm 118:8).
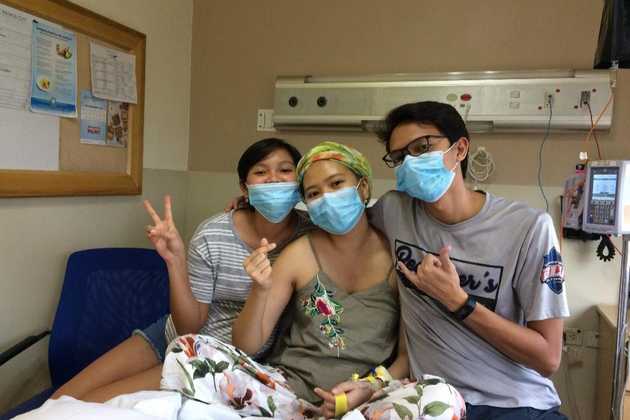
On September 3, I celebrated my 25th birthday. I was astounded with God’s love personified through family, friends, and even strangers. I prayed for providence, especially that treatment is financially challenging, and support has been pouring in from various people. I was grateful to Mr. Lemuel, my college clinical instructor, and to co-workers from Maria Reyna-Xavier University Hospital, Inc. who began fundraising. Colleagues from the Operating Room Nurses Association of the Philippines–Northern Mindanao Chapter and Xavier University Graduate School Student Council also reached out. I joined these organizations because I wanted to give and serve, hence I was overwhelmed to be at the receiving end. I prayed to the Lord to heal me so I can give back and pay it forward.
In the evening of September 6, a week before my scheduled fourth chemotherapy session, September 12, I was brought to the Emergency Room. My temperature upon arrival was 38.6°C. My WBC count was at only 0.60. I was having febrile neutropenia. I was again referred to the IDS, who started me on intravenous antibiotics and conducted blood and urine culture to detect infection as I reported pain in urinating the past weekend. I was also referred back to the dentist because of swollen gums. It was an extra stressful trip to the hospital as my sister was also admitted days after for acute gastroenteritis. I cannot imagine the burden of my parents having two sick children.
But, the mercy of the Lord is everlasting (Psalm 100:5). The illness of my sister was easily addressed and she was discharged after 3 days of confinement. I, on the other hand, was cleared from blood and urine infections; although I had another visit to the dental clinic for some procedures and my anticoagulant was again stopped for 48 hours prior and resumed a day after. I was also injected with GCSF twice to increase my WBC count and when it was at 4.60, I had my fourth chemotherapy session.
As I continue to receive chemotherapy, I ask the Lord for endurance. I pray that I may embody Christlike attitude in this difficult journey. I pray that others may see Him in my ordeal and recognize His presence in their lives.