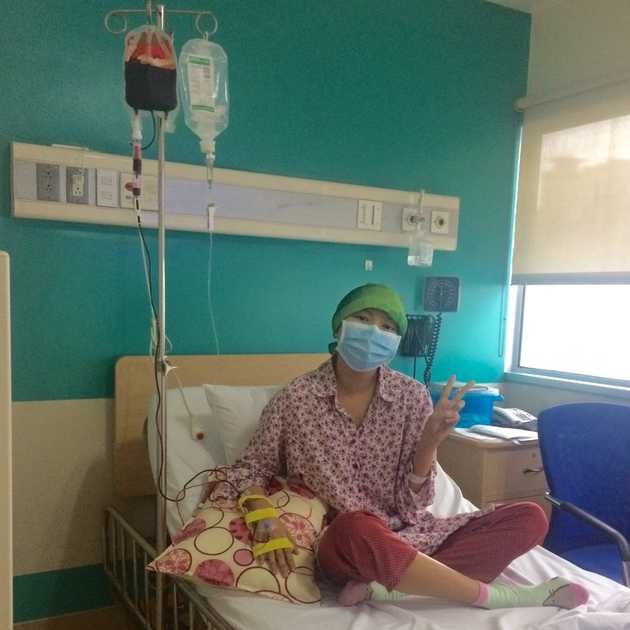
Ice Chips
November 01, 2018We always say that things get better. Well, let me tell you that chemotherapy is not one of those things. I hate chemotherapy. Still, I hate you more, cancer. Sure, good days eventually come but the bad days are excruciating not only in body but also in spirit.
On October 2, I went to the hospital for some blood works prior to my fifth chemotherapy session the following day. I actually felt good so I expected no complications this time, unlike the past four sessions where I had to stay in the hospital for several days. But, lo and behold—as I said, chemotherapy is not one of those things that get better—I needed blood transfusion and I was neutropenic again. These were some of my blood counts:
- Hemoglobin: 75 (Normal: 120-175 g/L)
- Hematocrit: 0.22 (Normal: 0.36-0.47)
- Red Blood Cell: 2.61 (Normal 4.20-5.40 x1012/L)
- White Blood Cell (WBC): 1.70 (Normal: 4.50-10.00 x109/L)
I was transfused with two bags of blood and to increase my WBC count, I was again injected with Granulocyte Colony Stimulating Factor.
On the night of October 3, a psychiatrist visited me and asked if she could conduct a survey for their study on the quality of life of cancer patients. Of course, I said yes. I was cheerful answering the questions. At the beginning, they were easy and matter-of-fact. Then, the questions turned difficult. But that is how interviews work, questions begin on the surface level and dive in deep. I was asked about hospice palliative care. There was that word again: palliative. And, it brought a friend: hospice. I was asked if I am receiving hospice palliative care and more. I was unsure how to answer even though there were options. Am I receiving this kind of care? I knew I was receiving treatment. I knew I am in an advanced stage. I refuse to say the last stage. I hate you, cancer. I knew that basically there is still no cure for cancer; although there are people that are on remission for years. I knew that hospice palliative care is the comfort provided to terminally-ill patients, the support given to improve the quality of life of dying patients, and the relief from pain of patients as they approach the end of life. And, I still hope I will be cancer-free after treatment. Hence, I was confused if I am receiving this kind of care. Still, I answered in good spirit. Then, she asked me, “How long do you think you will live?” I looked at the options and cried. It caught me off guard and broke my heart. I shared about my struggle between science and faith. As a nurse, I understood how science see illnesses. I understood how science see the numbers, the chances, the probabilities, and the statistics. But, I am not a statistic. I don’t want the length of my life determined by chances. I told her my faith simply tells me I will live. I looked at the options again and chose the longest option: 10 years and above. Take that, cancer. I wiped my tears and felt victorious. I just answered one question for a survey and it already felt like I punched cancer in the face.
A beautiful thing happened next. The psychiatrist reaffirmed my faith and told me that God loves me. I realized that she is a woman of faith. God sent me another person in the field of science who bears the same faith. We ended the interview by praying together. God really never ceases to amaze me.
On October 4, I had my fifth chemotherapy session. My oncologist scheduled my sixth on the 25th and then I will undergo CT scan after. She told me that depending on the results of the scan, we might consider radiation therapy next.
After I was discharged, the side effects of chemotherapy crushed my body and spirit for 6 days. I lost appetite. It was a struggle to force myself to eat. I was uncomfortable with my stomach. I was nauseous. I wanted to vomit but couldn’t. My mouth felt weird. Ice chips were a saving grace. I could not articulately describe the pain but I was begging the Lord to give me endurance. I asked Him to save me—save me even from my own mind and the battle in there. I asked Him to take away the fears and doubts.
When these dark days were over, I thought I could finally breathe and gather all my strength, hope, and faith for my sixth chemotherapy session. I did not know that I’ll be needing them sooner because just 4 days after, I had my scariest experience during this treatment yet.