Breathe
October 15, 2019Then the Lord God formed a man from the dust of the ground and breathed into his nostrils the breath of life, and the man became a living being. (Genesis 2:7)
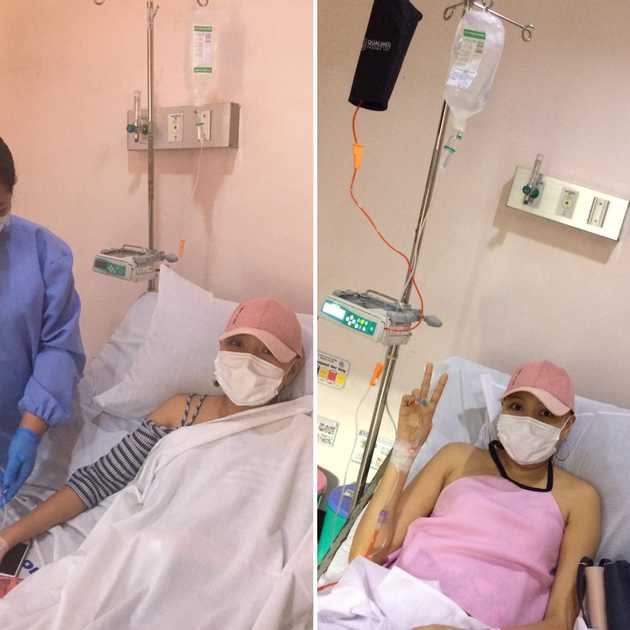
Breathe. Breathe. Breathe. That was all that I could think of as I gasp for air. I wanted to lash out but I couldn’t even cry because I know it will be more difficult to breathe. Would I take my last breath soon? God, would this be my earthly end?
Before my sudden health decline, I had an uneventful 3rd and 4th chemotherapy sessions. I also had my mid-treatment scans and though the results were not what I and my local oncologist wanted, we saw it as progress and decided to continue with the RCHOP protocol.
On June 22, I was admitted in the hospital. My WBC count was 0.5 (normal is 5.0-10.0). This was my first severe neutropenia episode in this protocol. I was given GCSF, antibiotics, and steroids. On June 26, I was discharged. But, only a few days after, I was once again admitted.
On July 1, I suddenly had trouble breathing. My doctors suspected hospital-acquired pneumonia due to my recent admission so I was started on antibiotics and was given oxygen support. However, my dyspnea (difficulty breathing) continued to worsen. I was gasping for air when I was upright and my chest felt heavy and tight. My doctors thought of pulmonary embolism (a blood clot in the lung) because I have chronic clots in my chest and neck. I was so scared because I knew that pulmonary embolism is deadly.
Praise Jesus! My test results were negative and my doctors ruled out pulmonary embolism.
But, I continued to be dyspneic. And, my blood pressure began to drop. I was started on norepinephrine (a drug to increase and stabilize the blood pressure) and soon was transferred to the intensive care unit (ICU).
I hated being in the ICU because it was lonely and it made the gravity of my situation more real. It was hard to convince myself that everything will be alright when I can see the patient across me on life support, when I know that the patient next to me coded and died. It disturbed my psyche, how I was once taking care of these patients and now I’m one of them fighting for my life too.
It was going downhill in the ICU. I started having premature ventricular contractions. It felt like my heart was going to jump out of my chest. My cardiac marker for heart failure was high. My chest CT scan read that the right ventricle of my heart is compressed by my inwardly-pressed chest bones, a condition called pectus excavatum, whose only treatment is surgical intervention.
I felt attacked and powerless. I badly wanted to cry but all I can think of is breathe; so there, I lay, attached to an oxygen support, hooked to an intravenous line, and had not shed a tear.
With the severity of my case, my family decided to bring me to Manila and I had to be airlifted.
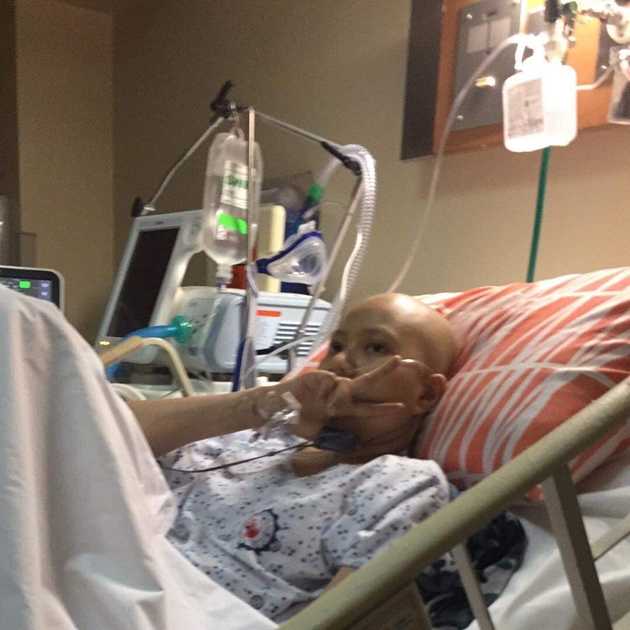
I arrived in the emergency room with a respiratory rate of more than 40 breaths per minute (normal is 12-20). The pulmonologist fellow said that I was breathing too fast and it may cause an arrest. She said that I may needed to be intubated and hooked to a mechanical ventilator if the BiPAP machine (a noninvasive ventilator that helps push air into the lungs) wouldn’t work. I didn’t want a tube down my throat so I prayed really hard. I tried really hard, even though it felt like I was drowning from the air pressure of the machine. I was so weak but I repeatedly thought that Christ is in me.
I was admitted in the progressive cardiac unit. Other doctors—cardiologist, thoracic surgeon, oncologist, interventional radiologist and infectious disease specialist—were also on board. I went through a lot of different tests and scans. Praise Jesus, I didn’t need surgery. My heart was okay. My cancer was also okay although my treatment had to be delayed. I was finally diagnosed with pneumocystis pneumonia, a severe form of pneumonia among the immunocompromised.
I was in the hospital for more than a month and about 3 weeks of that, I was bedridden. I had to be referred to the rehabilitation services to help me ambulate. It was not only physically tough but mentally, emotionally, and spiritually tougher. I finally cried when I was already in a regular room and could breathe better. I cried for the pain I caused my family. I cried for myself. And, I cried to the Lord Jesus Christ for the favor, for keeping me alive.
On August 7, I was discharged but few weeks later I was told that my cancer is refractory and the RCHOP protocol is not anymore working. Often, I don’t understand His plans but I hope I could grasp how wide and long and high and deep His love is for me.