Fire
December 02, 2019In all this you greatly rejoice, though now for a little while you may have had to suffer grief in all kinds of trials. These have come so that the proven genuineness of your faith—of greater worth than gold, which perishes even though refined by fire—may result in praise, glory and honor when Jesus Christ is revealed. (1 Peter 1:6-7)
Refractory. It is a word that no cancer patient want to hear. Also called resistant cancer, refractory cancer is one that does not respond to treatment. I was not responding to the RCHOP or RCVP (they had to remove a drug that was cardiotoxic because I already received its maximum lifetime dose) treatment protocol anymore. The tumor on my right kidney grew to be palpable. My oncologist recommended polatuzumab, a drug that was newly approved by the FDA in the US but is still not available in the Philippine market and can only be acquired through a compassionate program that would take weeks for approval.
For the mean time, I was referred to a urologist for a stent insertion in my right ureter to help preserve my right kidney while we wait. As an OR nurse, I had assisted such procedure and knew it would be quick. But I did not anticipate the postoperative pain. It hurt so much that days after discharge I went to the ER in the middle of the night. The pain lasted for around a week.
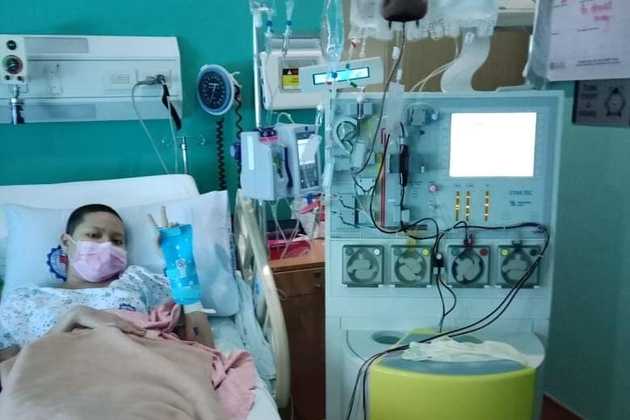
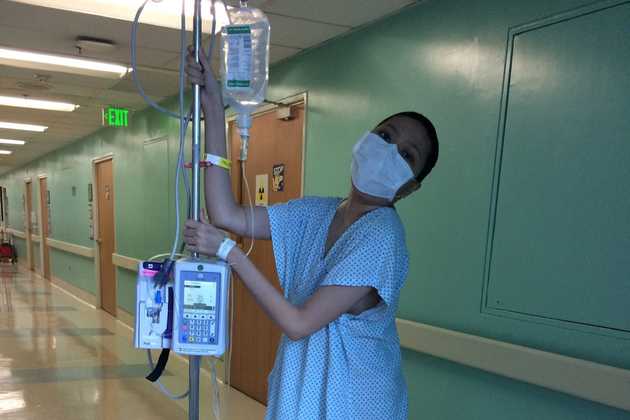
Weeks passed and the tumor on my right kidney grew to be protruding on my abdomen. Pain also began in my right abdomen and flank area. I could not wait for the polatuzumab anymore. I was referred to another oncologist, a stem cell transplant expert. He recommended various treatment protocols to hopefully bring me to remission and make me eligible for a stem cell transplant, which would hopefully keep me in remission longer. On September 22, I was admitted. The following 2 days, I underwent stem cell harvesting through a femoral vein access (right groin).
After the harvesting, I had my first cycle of my third treatment protocol: two intravenous drugs, obinutuzumab and bendamustine, and one oral drug, ibrutinib. I had to stay in the hospital longer because the first infusion of obinutuzumab was given in 3 weeks. The drugs were infused through another femoral vein access (left groin) as the first one was immediately removed and an attempt for an internal jugular vein access (right neck) failed. All was done in the bedside and under a local anesthesia. The insertion hurt, but the removal did not.
I also needed blood transfusion, electrolyte correction, and even a bronchoscopy lavage to identify possible infections that might had been causing my fever and cough. The fever was eventually identified as malignant in origin. I was discharged on October 13.
On October 31 and November 1, I had another hospital stay for my second cycle. And, on November 22, I underwent a PET/CT scan.
I received the result electronically on the night of November 25. It immediately brought me to tears. My disease progressed! It progressed on my mediastinum, on my lungs, on my kidneys, and on my aorta. I cried over frustrations. What options do I have now for treatment? How long will it be? What side effects do I have to endure? I cried for my family. How long do I have to burden them? How long do they have to be in pain, in anxiety, in fear? How long do they need to make ends meet? I cried to God. Why? Why this mountain? Why this giant? Why this fire? Do I lack faith?
I am still refractory, still resistant. But, I still have that quiet confidence in the deepest recesses of my heart that God will heal me. I may not fully understand God but I know He is with me in this fire and me in this fire will bring glory to Him as written in the verse above.